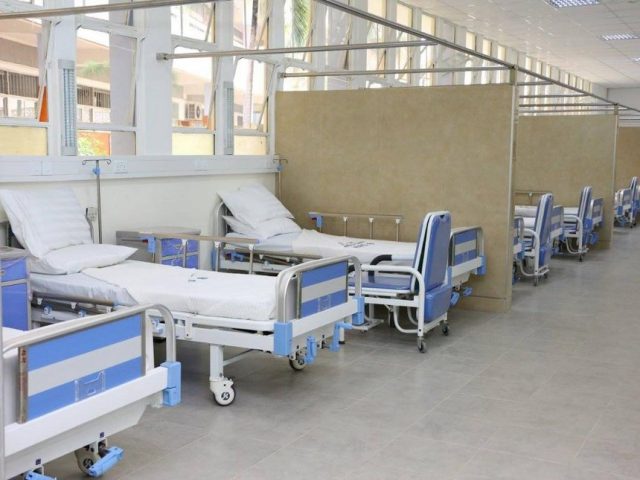
As COVID-19 takes a toll on Kenya’s healthcare systems, insurers are careful not to plunge into debt in the name of paying for COVID-19 medical expenses for their policyholders. They have adopted a measure that will force those insured to dig into their pockets when seek healthcare from specific health institutions.
Insurance companies have adopted a proposal to drop coverage for COVID-19 treatment in private institutions to cut down on expenses related to the respiratory disease that could push them into losses. Instead, they will only foot bills for coronavirus disease treatment in public hospitals. According to Business Daily, the Insurance regulator told the Senate that insurance companies will not pay for treatment in private hospitals where bills range from Sh600,000 to Sh1.2 million. But they will cover expenses incurred in public hospitals where bills for treatment of the infectious virus are estimated at Sh135,000.
“The insurance industry will pay for testing and treatment offered in government hospitals. These will include facilities run by the central government and county governments. Persons treated in private hospitals will be requested to make their own arrangements,” said Godfrey Kiptum, the IRA chief executive.
Insurance companies have received claims amounting to Ksh11.9 million since COVID-19 was reported in the country. So far only Ksh1.45 million has been paid out. The number of claims will keep rising if COVID-19 persists. In this COVID-19 pandemic, the regulator has inclined more towards the welfare of policyholders, by reviewing some of the rules. For instance, late filing of claims or failure to pay premiums will not be used as an excuse to avoid coronavirus-related claims.



